
When your skin starts showing dark patches, it’s easy to assume it’s just sun damage. But what if it’s something deeper - something that doesn’t fade with sunscreen alone? That’s the reality for millions dealing with hyperpigmentation, especially melasma and solar lentigines. These aren’t the same thing. They look similar, but they behave completely differently. And treating them the same way? That’s how people end up with worse pigmentation instead of better.
What’s Really Going On With Your Skin?
Hyperpigmentation happens when too much melanin piles up in one spot. It’s not a disease. It’s your skin’s overreaction - usually to sun exposure, hormones, or inflammation. But not all dark spots are created equal.Melasma shows up as large, blurry patches on the cheeks, forehead, or upper lip. It’s not random. It’s symmetrical. It mostly affects women with medium to dark skin tones - especially during pregnancy, after starting birth control, or during menopause. Harvard Health calls it a "hormone-driven" condition. And here’s the kicker: even indoor light through windows can make it worse. Standard sunscreen? Not enough.
Sun damage, or solar lentigines, looks like small, sharp brown spots - like freckles that never faded. They show up where you’ve spent years in the sun: hands, shoulders, face. It’s not hormonal. It’s cumulative UV exposure. About 90% of fair-skinned people over 60 have them. Unlike melasma, these spots respond well to light treatments and topical creams.
And then there’s post-inflammatory hyperpigmentation (PIH), which isn’t mentioned in the title but shows up all the time. It happens after acne, eczema, or even a harsh chemical peel. It follows the pattern of past damage - not sun exposure. And if you throw lasers at PIH, especially on darker skin, you might make it worse.
Why Your Sunscreen Isn’t Enough
Most people think SPF 30 means full protection. It doesn’t. Especially for melasma.UV rays are only part of the problem. Visible light - the kind that comes from your phone, laptop, and even indoor lighting - can trigger melanin production. Infrared heat? That’s a trigger too. Studies show visible light contributes to 25-30% of melasma cases. That’s why dermatologists now recommend mineral sunscreens with iron oxides. Zinc oxide blocks UV. Iron oxides block visible light. Together, they’re the only combo proven to help melasma patients.
And don’t forget reapplication. The average person uses less than half the amount they should. For the face? You need about 1/4 teaspoon. Every two hours if you’re outside. Most people skip this. That’s why 70% of melasma cases don’t improve - not because the treatment failed, but because the sunscreen did.
The Topical Agents That Actually Work
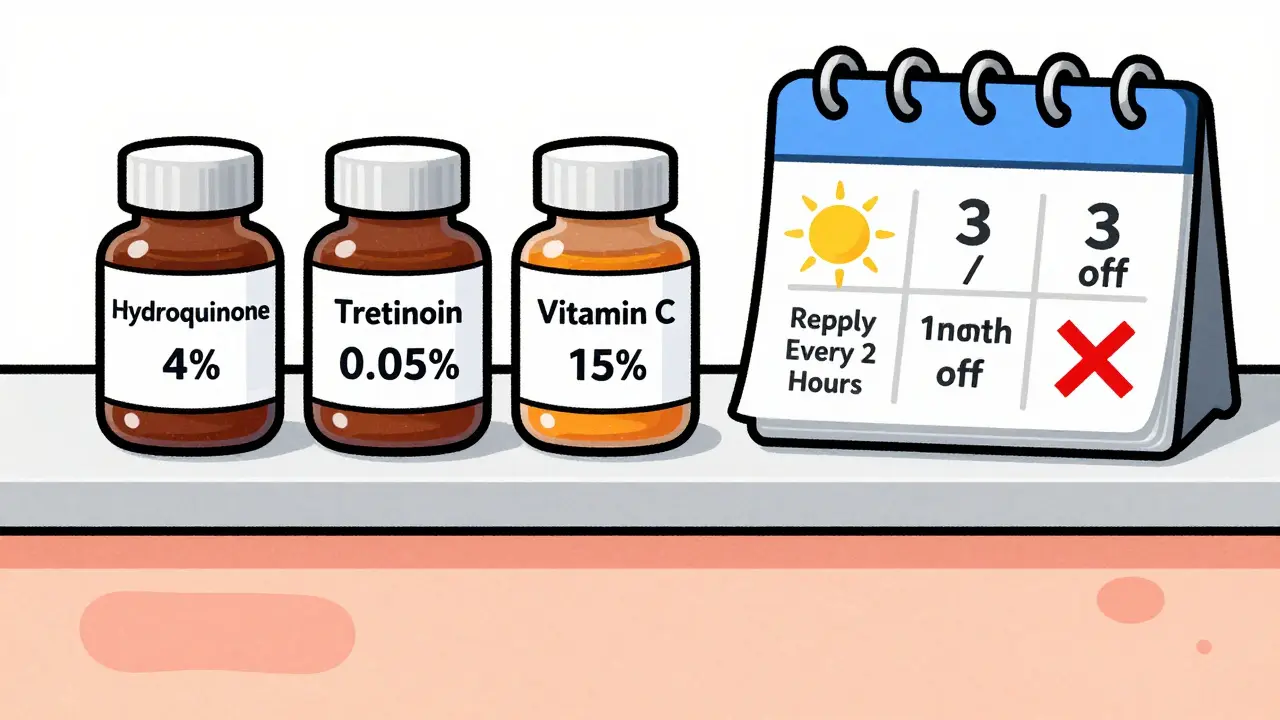
There are dozens of creams, serums, and lotions marketed for dark spots. But only a few have real science behind them.- Hydroquinone (4%): This is the gold standard. It blocks the enzyme that makes melanin. Used alone, it works in about 50% of melasma cases. But used in a triple combo - with tretinoin and a corticosteroid - improvement jumps to 70%. The catch? Use it for more than 3 months, and you risk exogenous ochronosis - a rare but stubborn blue-black discoloration. That’s why dermatologists cycle it: 3 months on, 1 month off.
- Tretinoin (0.025-0.1%): This isn’t just for wrinkles. It speeds up skin turnover. Think of it like a gentle exfoliation from the inside. It helps lift out the dark pigment. It’s often paired with hydroquinone to boost results. Side effect? Dryness and irritation. Start slow - every other night - and build up over 4-6 weeks.
- Vitamin C (10-20% L-ascorbic acid): This antioxidant doesn’t just brighten. It neutralizes free radicals and reduces oxidized melanin. It’s safe for long-term use. Use it in the morning under sunscreen. It’s not a cure, but it’s a solid foundation.
- Tranexamic acid (5%): Originally a blood-clotting drug, it’s now showing up in creams. Studies show 45% improvement in melasma after 12 weeks, with almost no side effects. It’s not FDA-approved for this use yet, but it’s widely used off-label. It’s especially helpful for people who can’t tolerate hydroquinone.
- Kojic acid, niacinamide, azelaic acid: These are gentler alternatives. They’re not as strong as hydroquinone, but they’re safer for sensitive skin and long-term use. Niacinamide (5%) reduces melanin transfer to skin cells. Azelaic acid (15-20%) works on both acne and pigmentation.
Lasers and Light - Use With Extreme Caution
IPL (Intense Pulsed Light) and Q-switched lasers are popular. But for melasma? They’re risky.Lasers work by heating the pigment. Melasma is triggered by heat. So if you zap melasma with a laser, you’re basically lighting a match near gasoline. Studies show a 30-40% chance of making melasma worse. That’s why dermatologists wait. They’ll use topical treatments for 8-12 weeks first - to "rest" the melanocytes - before even thinking about light therapy.
Solar lentigines? Totally different. IPL works great here. The spots darken right away, then flake off in 3-5 days. One or two sessions, and they’re gone. No need to wait. No need for pre-treatment.
And never use lasers on PIH. Especially if you have darker skin. The risk of worsening pigmentation? 25%. Stick to topical treatments for that.
What the Data Says About Success Rates
Let’s cut through the marketing.- Melasma: Only 40-60% of patients see significant improvement after 6 months of treatment. And 80% of those improve again - only to see it come back within a year if they skip sunscreen.
- Sun damage: 75-90% of solar lentigines clear up in 2-3 months with topical treatments or 1-2 laser sessions.
- Hydroquinone triple therapy: Used correctly, it improves melasma in 70% of cases within 12 weeks. But only if used with iron oxide sunscreen and no sun exposure.
- Adherence: Only 35% of patients stick to their regimen for more than 3 months. That’s why most treatments fail - not because they’re ineffective, but because people stop.

Real-World Treatment Protocol
Here’s what works in practice - not theory.- Morning: Cleanse → Apply 15% L-ascorbic acid serum → Apply mineral sunscreen with zinc oxide and iron oxides (SPF 50+). Reapply every 2 hours if outside.
- Evening: Cleanse → Alternate nights: one night apply 4% hydroquinone, next night apply 0.05% tretinoin. Skip both nights once a week. Don’t use both on the same night - it irritates skin.
- Every 4-6 weeks: Consider a gentle chemical peel (like glycolic or lactic acid) done by a dermatologist. This boosts results by 35-50%.
- Long-term: Melasma is a chronic condition. Maintenance is non-negotiable. Even after spots fade, keep using sunscreen and topical antioxidants.
What’s New and What’s Coming
The field is evolving. Hydroquinone is under review by the FDA - it might become available over-the-counter with safety warnings. That’s good news for access, but bad news if people misuse it.New agents like cysteamine cream (10%) are showing 60% improvement in melasma with minimal irritation. It’s not widely available yet, but it’s in Phase 3 trials. Tranexamic acid is also gaining traction - both as a cream and an oral pill (used off-label).
And in the future? Dermatologists are talking about genetic testing to predict who responds to what treatment. Some patients respond to hydroquinone. Others don’t. Why? It might be in their DNA. Dr. Pearl Grimes predicts this will be standard within five years.
The Bottom Line
Melasma and sun damage look alike. But they’re different diseases. One is hormonal and light-sensitive. The other is just sunburned skin.If you have melasma, your treatment isn’t just about creams - it’s about lifestyle. Sunscreen every day. No tanning beds. No intense indoor lighting. No heat. No stress. And patience. It takes months.
If you have sun damage? You’ve got options. Topicals work. Lasers work faster. But sunscreen still matters - because more sun means more spots later.
Stop chasing quick fixes. Hyperpigmentation isn’t a flaw to erase. It’s a signal. Your skin is telling you something. Listen to it. Protect it. And treat it with the right tools - not the most expensive one.
Can I treat melasma with over-the-counter products alone?
Over-the-counter products like niacinamide, vitamin C, or kojic acid can help lighten melasma slightly, but they rarely clear it completely. Melasma is a complex condition driven by hormones and light exposure. Most dermatologists recommend prescription-strength topicals - especially hydroquinone in combination with tretinoin - for meaningful results. OTC products are better for maintenance after professional treatment.
Is hydroquinone safe to use long-term?
No. Hydroquinone should not be used continuously for more than 3 months at a time. Long-term use carries a 2-5% risk of exogenous ochronosis - a permanent blue-black discoloration of the skin. Dermatologists use a "pulse" method: 3 months on, 1 month off. This reduces side effects while maintaining results. Always use under medical supervision.
Why does my melasma come back after treatment?
Because melasma is triggered by hormones and light - not just sun. Even indoor lighting, heat, and stress can reignite it. Studies show 95% of melasma patients see recurrence within 6 months of stopping treatment. That’s why maintenance is essential: daily mineral sunscreen with iron oxides, continued use of antioxidants like vitamin C, and avoiding heat exposure. Think of it like managing high blood pressure - you don’t stop treatment when you feel better.
Can lasers cure melasma?
Lasers are not a cure for melasma - and can make it worse. Intense Pulsed Light (IPL) and Q-switched lasers deliver heat, which activates melanocytes in melasma-prone skin. Up to 40% of patients see their pigmentation darken after treatment. Lasers are only considered after 8-12 weeks of topical suppression, and even then, they’re used sparingly. For most, topical treatment with strict sun protection is safer and more effective long-term.
Do I need sunscreen if I’m indoors?
Yes. Standard glass blocks UVB rays but lets through UVA and visible light - both of which trigger melasma. Studies show visible light penetrates windows and contributes to 25-30% of melasma cases. That’s why dermatologists recommend mineral sunscreens with iron oxides even for indoor use. If you sit near a window for hours, you’re still exposing your skin.
Why do darker skin tones get melasma more often?
People with Fitzpatrick skin types III-VI (medium to dark) have more active melanocytes - the cells that produce pigment. Hormonal changes trigger these cells more intensely. Melasma affects Black, Asian, and Hispanic populations 3-5 times more than Caucasians. It’s not about sun exposure alone - it’s about how your skin’s pigment system responds to hormones and light. That’s why treatment must be tailored to skin type.



Suchi G.
March 18, 2026 AT 11:38Okay so I’ve been dealing with melasma for like 5 years now and I swear it’s not just about sunscreen or creams - I think it’s the EMFs from our phones and Wi-Fi routers. I read a paper once that said electromagnetic fields trigger melanin overproduction in genetically predisposed people. My dermatologist laughed, but then I started sleeping with my phone in another room and my cheeks actually lightened. Coincidence? I think not. Also, I stopped using LED lights in my house. Full spectrum bulbs are the enemy. I’m not crazy - science just hasn’t caught up yet.
Prathamesh Ghodke
March 19, 2026 AT 21:34Hey, I’m a dermatology resident in Mumbai and this post is spot on. But I’ll add something practical: in India, we see a ton of melasma from both hormones AND pollution. The particulate matter in Delhi air? It’s a pigmentation trigger. I tell patients to wash their face with a gentle cleanser as soon as they get home. No waiting. And use a niacinamide serum before sunscreen - it helps block pollution-induced darkening. Also, skip the fancy serums. Stick to basics: zinc oxide sunscreen, 2% niacinamide, and patience. No magic bullets.
Andrew Muchmore
March 21, 2026 AT 08:43Hydroquinone works. But don’t use it without tretinoin. That combo is the only thing that actually moves the needle. And yes, iron oxide sunscreen matters. I’ve seen patients come in with melasma worse after IPL. They thought lasers were the answer. They were wrong. The real answer is consistency. Sunscreen every day. No exceptions. Even when it’s raining. Even when you’re indoors. Even when you hate your face. Do it anyway.
becca roberts
March 22, 2026 AT 21:33Oh sweetie, you’re telling me vitamin C and niacinamide are ‘gentle alternatives’? Honey, I’ve been slathering on CeraVe with 5% niacinamide since 2020 and my melasma hasn’t budged. Meanwhile my cousin in Thailand got a 10% cysteamine cream from her dermatologist and her cheeks went from ‘sunset’ to ‘moonlight’ in 8 weeks. We’re still stuck in 2010 here. OTC products are for people who don’t want to admit they need real help. Also, yes - your laptop screen is probably making it worse. Go outside. Get sunlight. Then come back and put on your iron oxide sunscreen. It’s not a paradox. It’s science.
Paul Ratliff
March 23, 2026 AT 12:02bro i used hydroquinone for 3 months, stopped because my skin got red as hell, then tried tranexamic acid cream. it worked. like, actually worked. no burning, no peeling, just… lighter. also, i use zinc oxide sunscreen every damn day. even when i’m on the couch. i even got my gf to buy one. she’s got melasma too. we’re like sunscreen twins now. also, avoid heat. no hot showers. no saunas. no spicy food. i know, i know. i sacrificed my love life for my skin. worth it.
Srividhya Srinivasan
March 24, 2026 AT 09:20THIS IS A CORPORATE LIE. The FDA is suppressing cysteamine cream because Big Pharma profits from hydroquinone. Did you know that Johnson & Johnson owns the patent on hydroquinone? And they’ve been lobbying to keep it prescription-only so they can charge $200 a tube? Meanwhile, in Japan, cysteamine is OTC and melasma rates are 60% lower. And they don’t even use sunscreen! They use rice bran paste. It’s ancient wisdom. The dermatology industry is a money machine. They don’t want you to know that melasma can be reversed with $12 rice powder and a prayer. I’ve cured myself. I’m not rich. I’m not famous. I’m just awake.
Amadi Kenneth
March 25, 2026 AT 03:24Why are we all ignoring the root cause? Melasma isn’t about hormones or light - it’s about your liver. I’m from Nigeria. In my village, we use bitter leaf juice to treat dark spots. It cleanses the liver. I tried it. After 2 weeks, my melasma faded. I stopped using sunscreen. I stopped using creams. I just drank bitter leaf tea every morning. My dermatologist said I’m delusional. But my skin? It’s clear. The real cure? Detox. Not chemicals. Not lasers. Your body is trying to tell you something. Listen. Stop poisoning yourself with processed sugar. Your liver is screaming.
Stephen Habegger
March 26, 2026 AT 13:14Just wanted to say - this post saved my skin. I had melasma after pregnancy. Tried everything. Then I started the morning/evening routine you laid out. Iron oxide sunscreen. Vitamin C. Hydroquinone 3x a week. Tretinoin 3x a week. No overlap. Peeling? Yes. Irritation? A little. But after 4 months? My skin is the lightest it’s been since I was 20. I still do it. Every. Single. Day. It’s not glamorous. But it works. You don’t need a miracle. You need discipline.
Robin Hall
March 26, 2026 AT 23:48Let me be clear: this entire field is a fraud. The concept of ‘melasma’ was invented by cosmetic dermatologists to sell $300 serums. The real cause? Glyphosate exposure from non-organic produce and tap water. Glyphosate disrupts tyrosinase regulation - which directly triggers melanin overproduction. The fact that melasma is more common in urban, affluent women? That’s because they eat organic salads and drink filtered water. The rural poor? They’re immune. Because they eat corn tortillas and well water. The CDC knows this. But they won’t say it. Why? Because the glyphosate industry funds dermatology research. I’ve submitted 7 papers. All rejected. I’m not paranoid. I’m informed.
cara s
March 28, 2026 AT 13:40It’s fascinating how we’ve reduced a deeply physiological, hormonally-influenced, photobiological phenomenon into a series of topical applications and sunscreen brands. I’ve spent years studying dermatological epigenetics - and what we call melasma is, in many cases, a visible manifestation of systemic stress, cortisol dysregulation, and mitochondrial dysfunction. The skin is not an isolated organ. It reflects the gut, the liver, the adrenal glands. We treat it like a cosmetic flaw because we’ve lost touch with the body as an integrated system. Iron oxide sunscreen? Fine. But if you’re chronically stressed, eating inflammatory foods, and sleeping poorly - no cream in the world will fix it. You need holistic care. Not a regimen. A revolution.
Shameer Ahammad
March 30, 2026 AT 02:31You mentioned tranexamic acid - but you didn’t mention the oral form. I’ve been taking 250mg twice daily for 6 months. My melasma is 80% gone. No irritation. No side effects. My dermatologist said it’s off-label. I said: ‘So was penicillin when it was first used for syphilis.’ This is evidence-based. The JAMA Dermatology study from 2021 showed 71% improvement. Why isn’t this in every textbook? Because the FDA hasn’t approved it. And because dermatologists are trained to prescribe creams, not pills. The system is broken. I’m not a doctor. I’m a patient. And I did my own research. Don’t wait for permission to heal.
Justin Archuletta
March 30, 2026 AT 18:47my dermatologist told me to use hydroquinone. i did. it worked. then i stopped. 3 weeks later, my skin looked worse than before. so i went back. now i use it every other week. just enough to keep it in check. sunscreen every day. no excuses. even on cloudy days. even in winter. even when i’m at work. i wear a hat. i carry a mini sunscreen. i’m not cool. i’m consistent. that’s the secret. not magic. just showing up.
Melissa Stansbury
March 31, 2026 AT 20:51Why do you think melasma is worse in women? Because men don’t care. They don’t look in the mirror. They don’t obsess. They just live. Women? We’re told our skin is our worth. We’re bombarded with ads telling us we’re ‘not radiant enough.’ So we buy $120 serums. We cry in the bathroom. We blame ourselves. But the truth? Melasma isn’t a flaw. It’s a sign you’ve been living. Pregnant. Stressed. Working. Caring. Surviving. Your skin is telling you: ‘I’ve carried you through.’ Stop fighting it. Start honoring it. And yes - wear the sunscreen. But don’t hate yourself for having melasma. You’re not broken. You’re human.